You took a full week off. You stayed off the course, stretched every morning, iced it at night. By Thursday it felt almost normal, so you headed out to Saddle Rock on Saturday for the first time in weeks.
Front nine? Great. You were striping it.
Then somewhere around the 13th hole — maybe it was that buried lie in the rough, or the awkward stance on the slope at 15 — you felt it. That familiar grab. That sharp, catching ache in your lower back, just to one side of your spine, that tells you the round is basically over even if your scorecard isn’t.
You finish the back nine anyway, because you’re a golfer and that’s what golfers do. But Sunday morning, you can barely get out of bed.
If this loop sounds exhaustingly familiar, there’s a good chance your lower back isn’t just “tight.” There’s a specific structure that takes a beating in the golf swing — and understanding it is the first step to actually breaking the cycle.
The Structure Nobody Talks About: Your Facet Joints
Most golfers have heard of disc herniations and sciatica. But facet joints? They rarely come up until they become a problem — and then they become a big problem.
Here’s a quick anatomy lesson that actually matters for your game:
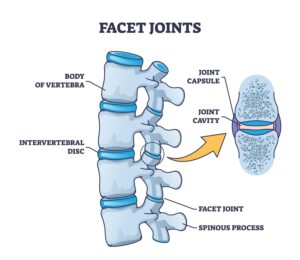
Running along the back of your spinal column are small, hinge-like joints called facet joints. They sit in pairs at every level of your spine and their job is to guide movement — letting you bend, rotate, and extend — while also acting as a brake to prevent you from moving too far in any one direction.
Now think about what a golf swing asks of those joints. You’re generating a rotational force through your lumbar spine at high speed, often repetitively for 18 holes, frequently with your back in slight extension at address and again through impact. That’s a lot of load on joints that, after 40, are already dealing with some natural wear.
When those joints become irritated, inflamed, or mechanically restricted, the result is Facet Joint Syndrome — and it produces a very specific set of symptoms that golfers describe almost identically:
- A sharp, “catching” sensation in the lower back, usually on one side
- Pain that’s worse when leaning back or rotating (follow-through)
- A deep ache that settles in after sitting in the cart or driving home
- Relief when bending forward, like at address — which is why the first few holes often feel fine
- Stiffness that’s worst in the morning and loosens up with movement
Sound familiar?
The Golf Swing Is Basically a Stress Test for Facet Joints
Here’s what makes golf particularly brutal for this condition: the swing doesn’t just load the facet joints — it loads them in exactly the wrong way.
Extension + Rotation = Facet Compression
At the top of your backswing, your lumbar spine is in extension and rotation simultaneously. That combination compresses the facet joints on the trailing side of your swing. Do that 80–100 (hopefully less) times in a round, often with poor hip mobility forcing your lower back to pick up the slack, and you have a very efficient recipe for irritation.
The Hip Mobility Connection
This is the part most golfers miss entirely. Research consistently shows that limited hip mobility — specifically a lack of hip rotation and extension — dramatically increases the mechanical load on the lumbar facet joints. When your hips can’t rotate freely through the swing, your lower back has to compensate. It hyperextends and over-rotates to create the power your hips aren’t contributing.
You’re not just dealing with a back problem. You’re dealing with a movement chain that’s been quietly failing you for a while.
The Cart Doesn’t Help
Extended sitting compresses the lumbar spine and inhibits the deep stabilizing muscles — specifically the multifidus, a small but critical muscle that attaches directly to each facet joint and helps protect it under load. The stop-and-start nature of a golf round — walk, sit in the cart, stand, explosive swing, sit again — keeps those muscles from ever properly warming up and staying warm.
When Can You Manage This Yourself?
Let’s be direct: not every facet flare-up requires a clinic visit. If you catch it early and the presentation is mild, a smart home protocol can interrupt the cycle before it becomes a chronic issue.
DIY is reasonable if:
- The pain stays localized in your lower back and does not travel into your glute, down your leg, or into your groin
- The onset was gradual — a long round, a weekend tournament, poor posture hunched over your phone in the cart
- It feels like a catch or stiffness, not a severe, locking spasm
- Bending forward gives you some relief
- You’ve had symptoms for fewer than 7–10 days
If you’re in that window, here’s a focused home protocol:
- Relative Rest (Not Total Rest) Stop the movements that force extension or heavy rotation — which means, yes, take a few days off the course. But don’t just lie on the couch. Movement is medicine here; it just needs to be the right movement.
- Flexion-Biased Mobility
- Child’s Pose — Hold 2–3 minutes. This gently opens the facet joint space, allowing synovial fluid to re-lubricate the area. Think of it as decompressing the joint.
- Cat-Cow — 15 slow reps, emphasizing the “cat” (rounding up) phase. Go very gently into the “cow” (dropping the belly) portion.
- Core Stabilization
- Dead Bugs — 3 sets of 10. This exercise trains your anterior core to control pelvic position, reducing the hyperextension your lower back is defaulting to. It’s not glamorous, but it directly addresses the compensation pattern driving your facet load.
- Hip Flexor and Thoracic Mobility Add a daily 90-second hip flexor stretch per side and some gentle thoracic rotation work. These two areas, when stiff, are often the hidden culprits forcing your lumbar spine to overwork.
- Ice, Then Heat Ice for the first 48 hours if it feels acutely sharp and inflamed. After that, switch to heat to relax the deep spinal muscles that are likely spasming to protect the irritated joint.
When DIY Isn’t Enough: The Red Flags
Stop your home protocol and seek professional assessment right away if you experience any of the following:
- Pain, numbness, or tingling that shoots into your leg or foot — This suggests nerve involvement and needs imaging and a proper diagnosis.
- Weakness in a leg, or foot drop — A neurological sign that requires urgent evaluation.
- Pain that woke you up from sleep — Night pain that’s positional-independent is a flag for something beyond simple joint irritation.
- The pain started after a fall, car accident, or significant impact — Trauma changes everything.
- You’ve done the DIY protocol for two full weeks with zero improvement — You’ve crossed the threshold. Time to get eyes on it.
The Gray Zone: Where Most Golfers Are Stuck
Here’s the honest truth about why you’re reading this article at all.
You’re probably not in severe pain. You’re not in the emergency room. You’re a 5/10 on a bad day, maybe a 2/10 on a good one. You can play — you just can’t play well. You’re gripping down on your irons. You’re shortening your backswing without realizing it. You’re compensating through the follow-through to avoid that catch. Your playing partners haven’t said anything, but your handicap is quietly telling the story.
This is what’s called the Gray Zone — and it’s where facet joint issues become chronic.
The problem with Gray Zone pain is that the DIY protocol provides just enough relief to get you back on the course, but not enough to actually fix the underlying movement problem. You feel 80%, go play, load the joints in the same dysfunctional pattern, and reset the clock on your recovery. Rinse and repeat, all season long.
The Gray Zone is almost always a sign that there is a biomechanical flaw — a movement compensation that no amount of child’s pose is going to resolve on its own. The joint keeps getting irritated because the root cause — restricted hips, poor thoracic mobility, a failing deep stabilization system — is still present and loading the same structure every time you swing.
This is where professional intervention stops being a luxury and starts being the most efficient path back to the golf you actually want to play.
What Professional Care Actually Looks Like for Golfers
Walking into a sports medicine or physical therapy clinic doesn’t mean you’re committing to months of passive treatment. For facet joint issues in active golfers, the best care is fast, targeted, and return-to-sport focused.
Here’s what a quality practitioner brings to the table that you simply can’t replicate at home:
Differential Diagnosis Facet joint pain, disc issues, and sacroiliac joint dysfunction all feel remarkably similar but require completely different treatments. Guessing wrong wastes weeks. A skilled clinician can determine the actual source of pain with a thorough assessment — often without needing imaging.
Biomechanical Assessment The real question isn’t just “what hurts” — it’s “why is this structure being overloaded?” A comprehensive movement screen will identify whether limited thoracic rotation, restricted hip mobility, or a failing deep core is forcing your lumbar facet joints to absorb forces they shouldn’t be absorbing. Treating the back without treating the hips is one of the most common reasons golfers stay stuck.
Spinal Manipulation or Joint Mobilization Targeted manual therapy can “gap” a restricted facet joint, restoring normal mechanics and often providing immediate pain relief. This isn’t about cracking your back — it’s about restoring the normal glide and movement of a joint that has become mechanically restricted.
Dry Needling The multifidus — the deep muscle that attaches directly to each facet joint — frequently goes into a protective spasm that surface-level treatments can’t reach. Dry needling can release these deep trigger points and interrupt the spasm-pain cycle quickly.
A Return-to-Golf Roadmap Perhaps most importantly, a good sports medicine provider doesn’t just get you out of pain. They give you a graded plan to safely reload your spine — building rotational power without re-irritating the joint — so you can get back to full swings, full rounds, and full confidence in your body.
The Bottom Line
Your lower back locking up every time you get back on the course isn’t just bad luck. It’s a signal. The rest-and-return loop you’ve been living in is telling you that something in your movement pattern is consistently overloading a specific structure in your lower back — and temporary rest is masking the problem without solving it.
If you’re fewer than 10 days into a mild flare, the home protocol above is a reasonable starting point. Work the flexion mobility, activate the core, stretch the hips, and give it two full weeks.
But if you’ve already been through that cycle more than once this season — if the pain keeps coming back every time you try to play — the most important thing you can do for your golf game is get an accurate diagnosis and a plan that actually addresses why this keeps happening.
The course isn’t going anywhere. But the longer a compensation pattern runs unchecked, the more deeply ingrained it becomes, and the longer the road back.
Dealing with a lower back that keeps flaring up every time you try to play?
- Schedule a movement assessment at Kinetic Sports Medicine & Rehab and find out what’s actually driving your pain — so you can stop managing symptoms and start playing full rounds again.
- Book Your Movement Assessment Here!
